Pain at Base of Skull When Touched: Causes and Treatments
Causes of Pain at the Base of the Skull
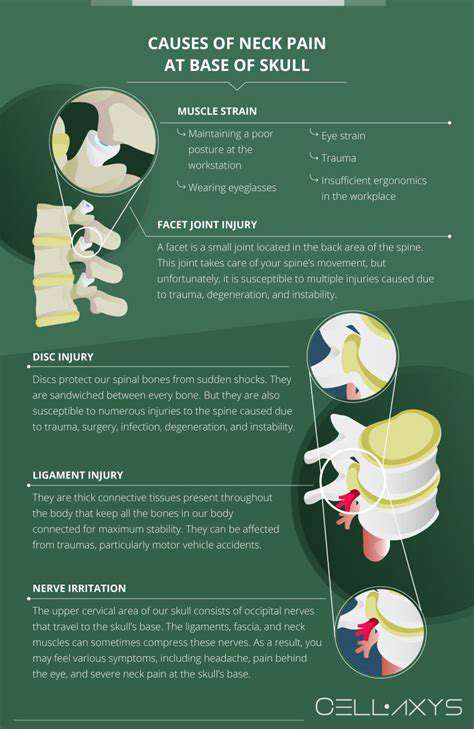
One of the most common reasons for experiencing pain at the base of the skull when touched stems from musculoskeletal problems. This encompasses a range of issues affecting the muscles, bones, and joints in the neck and upper back region. These issues often lead to referred pain, meaning the pain originates in one area but is felt in another, making it tricky to pinpoint the exact source initially. Poor posture, whether it's hunching over a computer, slumping on the couch, or habitually tilting the head, can strain the muscles, leading to tension headaches and localized pain at the base of the skull.
Furthermore, conditions like cervical spondylosis, which is age-related wear and tear affecting the spinal discs in the neck, can also trigger this type of pain. The degeneration of these discs can compress nerves or irritate the surrounding tissues, resulting in stiffness, tenderness, and throbbing sensations at the base of the skull. Additionally, muscle spasms in the trapezius or sternocleidomastoid muscles, common in individuals who experience significant stress, can contribute to this specific pain pattern. The intricate network of muscles in the neck makes it a prime target for tension and discomfort.
The presence of trigger points, which are hyperirritable spots within a tight band of muscle fiber, is another significant factor. These trigger points, when pressed or palpated, can cause localized or referred pain. In cases where there has been a recent injury, like whiplash from a car accident or a sports-related injury, the muscles and ligaments in the neck can become inflamed and sensitive, resulting in pain when touched at the base of the skull. Early intervention, such as physical therapy, can often alleviate these musculoskeletal issues and prevent them from becoming chronic problems.
Diagnostic procedures, such as palpation, may be used to identify specific areas of tenderness, or radiographic imaging, like X-rays or MRIs, may be performed to identify any structural abnormalities or damage to the cervical spine that could be contributing to the patient’s pain. Addressing the musculoskeletal causes requires addressing the underlying structural problems or the habits which have resulted in this type of pain. Lifestyle changes, such as improving posture and stress management, and the development of an exercise routine can dramatically help improve patient outcomes.
Neurological Factors and Nerve InvolvementNeurological factors can play a significant role in pain felt at the base of the skull, particularly when the area is touched. Nerve compression or irritation in the neck can lead to various pain patterns, including tenderness upon palpation. Occipital neuralgia, a condition characterized by inflammation or injury to the occipital nerves (nerves that run from the upper spinal cord through the scalp), is a common culprit. This condition can cause sharp, stabbing, or electric shock-like pain, along with a tenderness at the base of the skull.
Cranial nerve disorders can also be implicated, as some cranial nerves have branches that innervate the scalp and neck region. For example, the trigeminal nerve, which is the largest cranial nerve and responsible for sensation in the face, may sometimes cause referred pain to the base of the skull, especially if there is nerve compression or irritation. These problems can often lead to the development of secondary headaches.
Less commonly, more serious neurological conditions, such as tumors or infections affecting the brain or spinal cord, could lead to pain at the base of the skull. It is imperative that any neurological-related pain be treated promptly and with the correct approach. In such scenarios, the patient may also experience other symptoms, such as weakness, numbness, vision changes, or cognitive difficulties. If the neurological pain is accompanied by any other symptoms, it is extremely important to seek prompt medical attention.
Diagnostic assessments, such as neurological examinations and imaging studies (CT scans or MRIs of the brain and cervical spine), are essential to identify the underlying cause of the neurological symptoms. Treatment for neurological causes will depend on the diagnosis. This could involve medications to manage pain, nerve blocks to reduce nerve inflammation, or, in some cases, surgical interventions to relieve nerve compression or address structural abnormalities within the spine. A proper differential diagnosis is essential for ensuring the appropriate treatment path and an improved quality of life for the patient.
Systemic Conditions and Referred Pain PatternsSystemic conditions, affecting the entire body, can sometimes manifest as pain at the base of the skull. While less common, underlying conditions that trigger inflammation or affect the body's overall health can cause referred pain to the neck and head. For instance, certain types of arthritis, such as rheumatoid arthritis or osteoarthritis, can impact the cervical spine and cause pain and stiffness. These can, in turn, cause radiating pain in the neck and head, especially if the area at the base of the skull is touched.
Fibromyalgia, a chronic condition characterized by widespread musculoskeletal pain, fatigue, and tenderness in specific points, may also be associated with pain at the base of the skull. The tender points associated with fibromyalgia can easily be felt when palpating the back of the head. Some other underlying medical conditions, such as infections or autoimmune disorders, can cause inflammation that contributes to this type of pain. Identifying these systemic conditions requires thorough medical evaluations, including blood tests and imaging studies, to rule out serious underlying problems.
In some cases, even dental problems, such as temporomandibular joint (TMJ) disorders, can lead to referred pain in the head and neck region. The TMJ is a complex joint located near the ears, and dysfunction in this joint may radiate pain to nearby structures. Headaches can also radiate and be perceived as pain at the base of the skull. These types of headaches are often related to tension, stress, or the misuse of the neck muscles.
Management of systemic causes depends on the underlying diagnosis and the appropriate treatments of the systemic condition. This could include medications, lifestyle adjustments, physical therapy, or, in some cases, surgical interventions to address structural problems. In some cases, simply reducing your stress or modifying your sleeping position may provide substantial relief. A multidisciplinary approach involving various specialists is often necessary for effective diagnosis and comprehensive management of systemic conditions that cause pain at the base of the skull.
Treatment and Management Strategies
Identifying the Root Causes of Occipital Pain
Pain experienced at the base of the skull, often triggered by touch, can stem from a variety of underlying conditions, making accurate diagnosis the crucial first step in effective treatment. These potential causes can range from relatively benign muscle tension headaches to more serious issues like nerve compression or even, in rare instances, underlying structural problems affecting the cervical spine or the brain itself, thereby demanding a comprehensive approach to investigation. This detailed exploration is the foundation for a targeted treatment plan to alleviate discomfort and address the root cause of the pain felt at the base of the skull.
One of the most common culprits behind occipital pain is tension-type headache, frequently linked to stress, poor posture, and prolonged periods spent in static positions, such as sitting at a computer or driving. These headaches manifest as a tightening sensation in the neck and head, often presenting with tenderness upon palpation of the muscles at the base of the skull, where physical examination plays a pivotal role in differentiating from other pain sources. These aspects should be closely observed and well-documented.
Cervicogenic headaches, another significant source of occipital pain, originate from problems within the cervical spine, typically involving the joints, ligaments, or nerves of the neck. This can be caused by a sudden injury, such as whiplash, or chronic wear and tear, or even underlying inflammatory conditions, thereby disrupting normal function and transmitting pain signals to the occipital region, which is responsible for pain in the base of the skull. The identification and treatment of cervical spine issues are crucial for long-term pain management.
Occipital neuralgia, characterized by sharp, shooting, or electric shock-like pain along the occipital nerves, also contributes to the pain experienced when touched at the base of the skull. This condition occurs when these nerves, which run from the top of the spinal cord up through the scalp, become compressed or irritated, sending erratic pain signals. The underlying cause of the nerve irritation can range from muscle tightness to direct nerve damage, thereby prompting a detailed neurological assessment to be done to uncover the root cause of the issue.
Furthermore, less common but important causes to consider include inflammatory conditions like giant cell arteritis, a serious vascular condition that can also present with headaches, and, in exceedingly rare instances, tumors or other space-occupying lesions in the posterior fossa. A thorough medical history, including details about the onset, duration, and characteristics of the pain, in addition to a meticulous physical examination and potentially imaging studies, are essential for differentiating the various possibilities and determining the best course of action.
Conservative Treatment Approaches and Lifestyle Adjustments
For many individuals experiencing pain at the base of the skull, especially when the underlying cause is related to muscle tension or mild cervicogenic issues, conservative treatment approaches can offer significant relief and prevent the worsening of symptoms. These methods often involve a combination of lifestyle adjustments, self-care techniques, and physical therapies that are designed to address the root causes, reduce pain, and improve overall well-being. These efforts often provide the most effective and least invasive initial steps for managing pain and promoting healing.
Over-the-counter pain relievers, such as ibuprofen or acetaminophen, can provide temporary relief from pain and inflammation, allowing individuals to function more comfortably. These medications can be particularly helpful in managing headaches associated with muscle tension or mild nerve irritation, but prolonged use should be discussed with a healthcare professional to avoid potential side effects. However, the careful monitoring of the effects of these medications is important for patients, as well as the dosage instructions.
Heat and cold therapy can be beneficial in managing pain and muscle spasms. Applying a warm compress or taking a warm bath can help to relax tense muscles and improve blood flow, reducing pain and stiffness. Conversely, applying a cold pack can help to numb the area, reduce inflammation, and alleviate pain, making it particularly useful for acute pain. Regular use and variation of these treatments, tailored to the individual's response, may significantly improve comfort and reduce pain.
Physical therapy plays a crucial role in addressing musculoskeletal issues that contribute to occipital pain. A physical therapist can teach patients proper posture, ergonomic principles, and exercises to strengthen the neck muscles and improve range of motion. Additionally, manual therapy techniques, such as massage and mobilization, can help to release muscle tension, reduce nerve compression, and restore normal joint function, which is instrumental in the long-term management of the problem. Furthermore, this promotes enhanced posture and movement.
Lifestyle adjustments, such as improving posture, taking regular breaks from prolonged sitting, and managing stress levels, are also crucial for preventing and managing occipital pain. Practicing relaxation techniques, such as deep breathing exercises or meditation, can help to reduce muscle tension and improve overall well-being. Adequate sleep, a healthy diet, and regular exercise also contribute to reducing the frequency and severity of headaches and other pain conditions, positively impacting long-term outcomes.
Medical Interventions and Advanced Therapies
When conservative treatments fail to provide adequate relief for pain at the base of the skull, or when the underlying cause is more complex, medical interventions and advanced therapies may become necessary. These options, which range from medication adjustments to minimally invasive procedures, are designed to address specific causes, such as nerve compression, inflammation, or other underlying conditions. The selection of an appropriate intervention depends heavily on an accurate diagnosis and the individual's specific needs and medical history.
Prescription medications, such as muscle relaxants, nerve pain medications, or anti-inflammatory drugs, may be used to manage pain and reduce inflammation when over-the-counter medications are ineffective. These medications are often used to target specific pain pathways or address underlying conditions, such as occipital neuralgia or cervicogenic headaches. The careful monitoring of the effects of these medications by medical professionals is important for patients, as well as the dosage instructions.
Nerve blocks involve injecting a local anesthetic and sometimes a corticosteroid near the occipital nerves to block pain signals. These injections can provide both diagnostic and therapeutic benefits, helping to identify the source of the pain and provide temporary or long-lasting relief. Multiple nerve blocks might be necessary, and the use of imaging guidance can improve the accuracy and effectiveness of the injections, making them a valuable intervention for specific nerve-related pain.
Radiofrequency ablation (RFA) is a minimally invasive procedure that uses radiofrequency energy to damage the occipital nerves, thereby interrupting the transmission of pain signals. This procedure is typically considered when nerve blocks provide significant but temporary relief, offering a longer-lasting solution for managing chronic pain. Careful patient selection is key to achieving optimal outcomes, and post-procedure care is essential for proper recovery and pain management.
In rare cases, when other treatments are unsuccessful, surgery may be considered to address underlying structural problems or nerve compression. Surgical options may include procedures to decompress the occipital nerves or to stabilize the cervical spine. However, surgery is usually reserved for specific indications after a comprehensive evaluation and is often considered the last resort when all other therapies have failed to provide adequate relief. The risks and benefits of surgical intervention need to be carefully evaluated.
Preventive Measures and Long-Term Management
Preventing the recurrence of pain at the base of the skull, or at least minimizing its frequency and severity, involves adopting a comprehensive approach that combines lifestyle modifications, ergonomic adjustments, and proactive self-care practices. By implementing these strategies consistently, individuals can significantly reduce their risk of developing or experiencing recurring episodes of occipital pain, which can have a notable impact on their quality of life. Such measures require a long-term commitment.
Maintaining good posture is essential for preventing muscle strain and nerve compression, particularly when performing activities that involve prolonged sitting, such as working at a computer. Ensuring that the workstation is ergonomically correct, with the monitor at eye level, the keyboard and mouse within easy reach, and proper back support, can help to prevent neck and shoulder strain, significantly reducing the risk of developing occipital pain. These considerations should be kept top of mind.
Regular exercise, particularly activities that strengthen the neck muscles, improve flexibility, and promote overall cardiovascular health, can help to prevent the development of occipital pain. Exercises such as neck stretches, shoulder rolls, and gentle range-of-motion exercises are particularly beneficial. Incorporating these exercises into a daily routine can help to maintain good posture and reduce muscle tension. Furthermore, consistency is key for long-term benefits.
Managing stress through relaxation techniques, mindfulness practices, and adequate sleep is also crucial for preventing and controlling pain episodes. Stress can trigger muscle tension and exacerbate pain, which highlights the importance of incorporating stress-reducing techniques into daily life. Deep breathing exercises, meditation, and yoga are highly effective. Proper sleep hygiene is also necessary to improve your quality of life and prevent the recurrence of pain.
Regular medical check-ups and open communication with a healthcare provider are important for long-term management of occipital pain. Individuals should report any new symptoms, changes in pain patterns, or worsening of existing symptoms to their physician promptly. Developing a strong patient-physician relationship can lead to early intervention and improved outcomes. Additionally, the health professional can offer guidance on the most appropriate treatments based on the patient's condition, providing further support in pain management.