Crown Head Pain: Causes, Symptoms, and Effective Treatments
Common Causes of Crown Head Pain
Muscle Tension and Stress
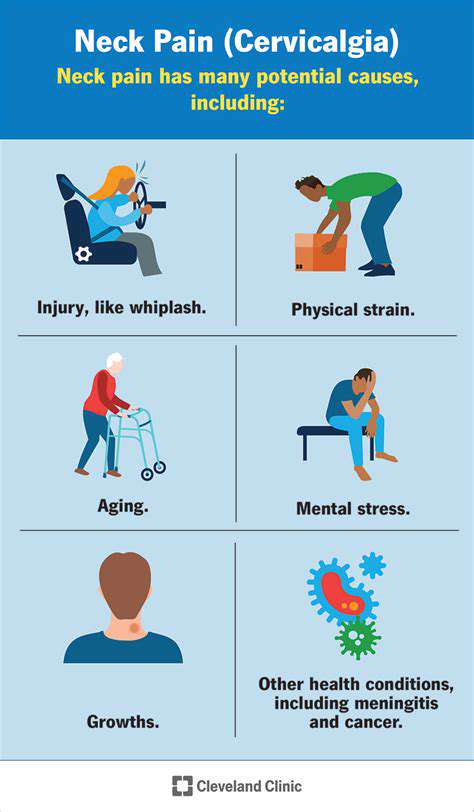
One of the most prevalent causes of crown head pain is the tension that arises from everyday stress and anxiety. These muscle contractions can particularly affect the muscles surrounding the scalp and neck, leading to a suffocating feeling. Individuals engaged in stressful occupations or those enduring personal crises often report a heightened sensitivity in the crown region of their heads.
Additionally, prolonged periods spent in poor posture—such as hunching over at a desk—can exacerbate muscle tension. When the neck and shoulders are strained, they can contribute significantly to the discomfort experienced at the crown of the head, leading to even more pronounced pain during physical activities or sudden movements.
Sinus Issues and Infections
Crown head pain can also manifest as a result of sinus problems, including sinusitis and allergies. When the sinuses become inflamed or infected, pressure can build up in the head, translating into pain that is often felt at the crown. This discomfort is frequently accompanied by other symptoms such as facial pressure, nasal congestion, or headaches concentrated around the forehead.
Recognizing sinus-related crown pain is crucial for effective treatment. Often, individuals may confuse sinus discomfort with tension headaches. However, understanding the distinct signs—like nasal blockage and facial swelling—can lead to more accurate diagnoses and prompt interventions to alleviate the pain.
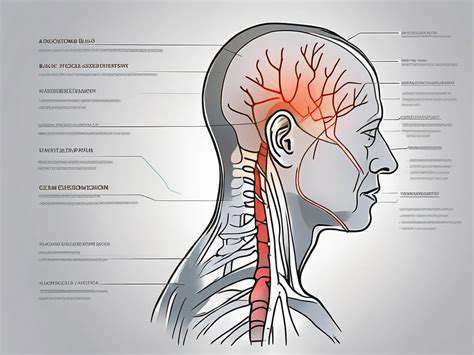
Neurological Conditions and Migraines
Crown head pain can be indicative of underlying neurological conditions, with migraines being a notable example. Migraines are known for their intense, throbbing pain, which can sometimes be localized to the crown or top part of the head. Accompanying symptoms such as nausea and sensitivity to light typically characterize these episodes, making them particularly debilitating for sufferers.
Other neurological conditions that might result in crown head pain include tension-type headaches and cluster headaches. Understanding one's headache patterns can empower individuals to seek appropriate medical advice and management strategies, leading to a better quality of life and reduced incidence of pain.
Identifying Symptoms Associated with Crown Head Pain
Common Symptoms of Crown Head Pain
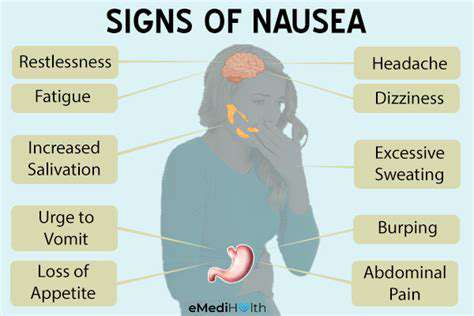
Crown head pain often presents with a variety of symptoms that can vary in intensity and duration. Understanding these symptoms is crucial for early identification and treatment. Some individuals may experience a throbbing sensation, while others report a consistent dull ache that can feel debilitating. Other symptoms may include sensitivity to light and sound, which can exacerbate the discomfort associated with crown head pain.
In addition to the pain itself, individuals may also notice accompanying effects such as nausea or dizziness. These additional symptoms can make it difficult to carry out daily activities, thereby impacting one's overall quality of life. Sometimes, crown head pain can be mistaken for tension headaches, which is why it’s essential to differentiate between the two through careful symptom identification.
How Symptoms Can Vary in Different Individuals
The presentation of crown head pain can significantly differ from one person to another, influenced by various factors such as genetics and environment. It’s not uncommon for someone to experience sharp, localized pain, while another feels a more widespread sensation of pressure. This variability signifies the necessity of a tailored approach when diagnosing and treating crown head pain.
Moreover, lifestyle habits, such as stress levels, sleeping patterns, and hydration, can also impact how symptoms manifest. For example, those who are frequently stressed may encounter symptoms more intensely, while individuals who practice regular relaxation techniques often report milder episodes. Understanding these differences can lead to more effective management strategies, enhancing the overall treatment experience.
Effective Treatments for Crown Head Pain
Understanding the Causes of Crown Head Pain
Crown head pain, also known as vertex headache, can stem from various underlying conditions. It's important to distinguish the origins of this pain to secure effective treatment. As tension builds in the muscles around the head, it can create a sensation that feels like a tight band squeezing down on the crown of your head. This pain can be incidental, caused by muscle strain or stress, or could signal deeper tension-related issues.
Another common cause of crown head pain is migraines, which often manifest with other symptoms such as nausea or light sensitivity. Migraines can be triggered by numerous factors including hormonal changes, environmental stimuli, or certain foods. Identifying these triggers is essential for both prevention and effective management of the condition. Keeping a headache diary can assist in tracking patterns that may exist over time.
Cluster headaches, while less common, also present significant pain that can focus on the crown area. They are periodic, often occurring in groups, hence the name. These headaches can be excruciating, often causing individuals to remain restless. Understanding the cyclical nature of cluster headaches can also provide insight into how and when to take preventive measures or medications for relief.
Medical conditions such as hypertension may also contribute to crown head pain. Elevated blood pressure can lead to tension and discomfort in the head due to increased pressure on blood vessels. Regular check-ups with a healthcare provider can help manage this and reduce the risk of more severe complications. Lifestyle changes, including dietary adjustments, can be an effective strategy for managing blood pressure-related head pain.
Finally, other factors such as sinusitis or even dehydration should not be overlooked. Sinus issues can lead to pressure build-up in the skull, while insufficient hydration can affect many bodily systems, including vascular health. Ensuring adequate fluid intake each day can help mitigate these risks and contribute to overall wellness, impacting crown head pain positively.
Effective Treatment Options for Crown Head Pain
When it comes to treating crown head pain, a multifaceted approach is often the most effective. Over-the-counter pain relievers such as ibuprofen or acetaminophen may provide immediate relief, especially for tension-type headaches. It is crucial to adhere to recommended dosages to avoid rebound headaches, which can occur with frequent use of these medications. Persistent users should consult a healthcare professional for advice tailored to their specific situation.
Additionally, cognitive-behavioral therapy (CBT) has garnered attention as an effective treatment modality for chronic pain, including crown head pain. This form of therapy addresses the mental and emotional aspects of pain, teaching individuals coping strategies that can significantly reduce their perception of pain. By reframing negative thought patterns, patients can learn to manage their symptoms better.
Physical therapies such as massage and chiropractic care can also be beneficial in alleviating crown head pain. These therapies target muscle tension, improving circulation and promoting relaxation. Regular sessions may not only relieve current pain but can prevent its recurrence by addressing the root causes such as posture deficiencies or muscle tightness that often contribute to crown pain.
In some cases, preventive treatments like prescription medication may be necessary, particularly for recurrent headaches or migraines. Consult with a healthcare provider who specializes in pain management or headache disorders. This specialist can tailor a treatment program that may include prescription medications or even alternative therapies that align with personal health goals.
Lastly, lifestyle modifications, such as incorporating regular exercise, maintaining a balanced diet, and practicing stress management techniques, can significantly impact the frequency and intensity of crown head pain. Activities such as yoga and mindfulness meditation provide comprehensive benefits, promoting both physical and mental health, thus contributing to a holistic treatment approach.