Back Head Nerve Pain: Possible Causes and Treatment Options
Table of contents
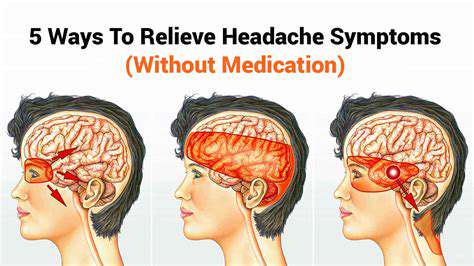
Tension-type headaches stem from muscle tension, causing back head nerve pain.
Occipital neuralgia leads to sharp pain from irritated occipital nerves.
Cervicogenic headaches result from cervical spine issues, causing referred pain.
Nerve compression syndromes pinch nerves, leading to localized pain and discomfort.
Understanding back head nerve pain aids in effective treatment planning and management.
Medications include NSAIDs and anticonvulsants for nerve pain relief.
Physical therapy focuses on strengthening muscles and improving flexibility for relief.
Alternative therapies like acupuncture and chiropractic adjustments help manage pain.
Seek professional help for persistent or worsening back head nerve pain.
Common Causes of Back Head Nerve Pain
1. Tension-Type Headaches
Tension-type headaches are often caused by muscle tension in the neck and scalp. Stressful situations or prolonged periods of poor posture can lead to tightness in these areas, contributing to nerve pain. Understanding the relationship between muscle tension and headache pain is crucial for effective treatment. Common symptoms include a dull, aching sensation and increased sensitivity around the head.
These headaches may radiate to the back of the head, causing discomfort that could affect daily activities. While they can occur at any age, they are particularly prevalent in adults who face high levels of stress or engage in repetitive motions. It is important to identify triggers to help prevent these episodes from becoming chronic.
Simple lifestyle modifications, such as regular exercise and practicing relaxation techniques, can significantly alleviate symptoms. Over-the-counter pain relievers may provide temporary relief; however, it's advisable to consult with a healthcare provider for persistent pain. By addressing the underlying factors contributing to tension-type headaches, individuals can improve their quality of life significantly.
2. Occipital Neuralgia
Occipital neuralgia is a condition characterized by inflammation or irritation of the occipital nerves. This often results in sharp, shooting pain at the back of the head and neck, making it challenging for affected individuals to focus on everyday tasks. It’s essential to recognize the symptoms early for effective management. This type of nerve pain may stem from trauma, muscle tightness, or underlying medical conditions.
Individuals with occipital neuralgia may also experience tenderness in the scalp, as well as throbbing pain that intensifies with movement. Diagnosis usually involves a thorough clinical evaluation, often complemented by imaging studies to rule out other potential issues. Treatment options may include medications, physical therapy, or even nerve blocks to alleviate pain.
With proper management, many can experience significant relief and a return to normal daily activities. It is advisable for those affected to maintain open communication with healthcare providers to tailor an effective treatment plan that suits their specific needs. From lifestyle adjustments to medical interventions, individuals have various avenues to explore in managing occipital neuralgia pain.
3. Cervicogenic Headaches
Cervicogenic headaches arise from issues in the cervical spine or neck, often leading to referred pain in the back of the head. These headaches typically stem from cervical spine disorders, such as herniated discs or arthritis, which can irritate the nerves. Understanding the close connection between spine health and headache patterns is crucial for effective treatment and relief.
Symptoms can include pain that worsens with certain neck movements, as well as tenderness around the neck and shoulder areas. Patients may also experience visual disturbances or nausea, making it vital to differentiate cervicogenic headaches from migraines or tension-type headaches. This differentiation ensures that individuals receive the most suitable treatment for their specific condition.
Physical therapy often plays a pivotal role in managing cervicogenic headaches. Strengthening and stretching exercises can help alleviate stiffness and improve spinal alignment, thereby reducing pain. Additionally, healthcare practitioners may recommend alternative therapies, such as acupuncture or chiropractic adjustments, which can be effective complementary treatments.
4. Nerve Compression Syndromes
Nerve compression syndromes can lead to varying degrees of pain in the back of the head, particularly if nerves are pinched within the neck or spine. Conditions such as herniated discs or spinal stenosis may exert pressure on the nerves, causing discomfort. Recognizing the presence of nerve compression is essential to prevent chronic pain from developing.
Symptoms often include localized pain, numbness, or tingling sensations that radiate from the neck to the head. Alongside prescribed medication, lifestyle changes, including ergonomic adjustments and regular physical activity, can help ease pressure on affected nerves. When managed effectively, individuals may find significant relief from symptoms, allowing for a return to their normal routines.
Surgical interventions may be required in severe cases where conservative treatments fail to provide adequate relief. Consultation with a specialized healthcare provider becomes imperative to determine the most appropriate treatment plan based on individual symptoms. As understanding of these syndromes improves, so too do the options available for effective resolution and management of back head nerve pain.
Treatment Options for Back Head Nerve Pain
Understanding Back Head Nerve Pain
Back head nerve pain, often described as a sharp or throbbing sensation, can significantly impact daily life. Understanding the nature of this pain is crucial for effective treatment. Nerve pain can arise from various conditions, including herniated discs, migraines, or underlying nerve compression issues. Recognizing the symptoms can aid individuals in seeking prompt medical attention.
This type of pain frequently radiates from the back of the head toward the neck and scalp, creating discomfort that can affect concentration and quality of life. It may also manifest alongside other symptoms, such as dizziness or vision changes, making a comprehensive evaluation by a healthcare professional vital. Identifying the exact cause of the pain can lead to more targeted and efficient treatment options.
The anatomy of the head and neck is quite complex, with several nerves intermingling to transmit signals. Nerves like the occipital nerve often become inflamed or irritated, leading to significant discomfort. Understanding this anatomy helps healthcare providers diagnose and prioritize treatment options effectively, ensuring patients receive tailored care based on their unique presentations.
In some cases, a detailed examination, including imaging tests like MRIs or CT scans, may be required to pinpoint the exact source of the pain. It’s essential for individuals experiencing persistent nerve pain to consult with a healthcare provider to rule out serious conditions that might require immediate intervention. By addressing these issues early, patients can potentially avoid chronic pain scenarios.
Overall, awareness and knowledge about back head nerve pain pave the way for more effective management. Individuals can empower themselves with information to discuss concerns and experiences more openly with healthcare providers, fostering a collaborative approach to addressing this challenging condition.
Medication Options for Relief
Medication remains one of the primary strategies in managing back head nerve pain. Non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen, can effectively reduce inflammation and alleviate pain. These over-the-counter medications are often the first line of treatment for individuals experiencing mild to moderate discomfort.
For more severe pain, healthcare providers may prescribe stronger medications, such as corticosteroids, which can provide significant relief by reducing inflammation directly around the affected nerves. It’s important for patients to follow their medical provider's guidance when using these medications to avoid potential side effects or dependency issues.
Additionally, anticonvulsants and antidepressants have been found effective in managing nerve pain. Medications such as gabapentin or amitriptyline can help modulate nerve signals and ease symptoms, especially in cases where pain has escalated to chronic levels. Patients should discuss the potential benefits and side effects of these medications with their providers to make informed choices.
Topical treatments, such as lidocaine patches or capsaicin creams, offer alternative options for localized pain relief. These applications can numb the area or reduce pain sensation, providing comfort without systemic medication side effects. Individuals often find substantial relief using such treatments in conjunction with oral medications.
Finally, it’s critical to evaluate medication efficacy continually. Pain management often involves trial and error to find the most effective regimen. Regular follow-ups with a healthcare provider ensure that patients can adjust their treatment plans as needed, ultimately improving their quality of life.
Physical Therapy and Exercise Techniques
Physical therapy is a cornerstone of rehabilitation for individuals suffering from back head nerve pain. Specialized therapists can design personalized exercise regimens that focus on strengthening the muscles surrounding the neck and back. Improved muscle tone can lead to reduced pressure on nerves and alleviate discomfort experienced in the back of the head.
Stretching exercises play a vital role in enhancing flexibility. Rigorous stretches targeting the neck and upper back can help ease tension, ensure better postural alignment, and contribute to pain relief. Therapists often incorporate specific techniques such as cervical traction, which can relieve compression on nerves and alleviate symptoms over time.
In addition to physical exercise, modalities like heat and cold therapy may be integrated into treatment plans. Applying heat can promote blood circulation and enable tighter muscles to relax, while cold compresses can help minimize inflammation and numb sharp pain. Such therapies combined with physical therapy can create a comprehensive approach to treatment.
Educating patients about ergonomic practices in their daily lives is crucial. Understanding how to maintain proper posture, especially during prolonged activities like computer use or driving, helps prevent flare-ups, contributing to long-term relief. Occupational therapists often provide valuable insights into workplace ergonomics and adjustments to enhance comfort.
Ultimately, physical therapy coupled with appropriate exercises offers a proactive way to manage back head nerve pain. Patients who commit to these practices may find significant improvements in their symptoms and an enhanced ability to engage in daily activities with greater ease and comfort. Through consistent effort, individuals can pave their way towards recovery and a better quality of life.
Alternative Therapies and Their Effectiveness
In recent years, alternative therapies have garnered attention as viable options for back head nerve pain management. Treatments such as acupuncture have become popular, targeting specific points along the body to relieve pain and promote overall healing. Numerous studies indicate that acupuncture can help alleviate migraines and tension headaches, which may benefit individuals experiencing back head nerve pain.
Chiropractic adjustments represent another alternative approach. Chiropractors use manual manipulation of the spine and neck to ease tension, improve alignment, and potentially relieve nerve compression. Many patients report significant reductions in pain frequency and intensity after undergoing regular chiropractic sessions, making it a favored adjunct to traditional medical treatments.
Meditation and mindfulness practices are increasingly recognized for their positive impact on chronic pain management. These techniques promote relaxation and stress reduction, which can be essential when dealing with persistent pain issues. Mindfulness training helps individuals cultivate a more accepting attitude towards their pain, allowing for better coping mechanisms in daily life.
Another promising alternative therapy is biofeedback, which involves using electronic devices to monitor physiological functions. Patients learn to control pain responses consciously and develop techniques to manage pain levels effectively. As patients become aware of their body’s signals, they can implement strategies to prevent pain exacerbation.
Individuals exploring alternative therapies should always consult with their healthcare providers. While these treatments can complement traditional options, they should be considered as part of a comprehensive pain management strategy. Open communication about all aspects of care is essential for maximizing the benefits of diverse treatment modalities.
When to Seek Professional Help
Knowing when to seek professional help for back head nerve pain is crucial. Individuals should be vigilant for warning signs, such as persistent or worsening pain that does not resolve with home remedies. Additionally, symptoms accompanied by neurological changes, including difficulty speaking, weakness in limbs, or sudden vision issues, warrant immediate medical evaluation.
Consulting a healthcare professional is also advisable if pain interferes with daily activities or sleep patterns. Chronic discomfort can lead to significant lifestyle limitations and decrease overall well-being. By discussing symptoms openly, patients can work with providers to develop a targeted treatment strategy and explore underlying causes that may need addressing.
Healthcare providers may recommend a multi-faceted approach, including medications, physical therapy, or imaging tests, depending on the severity of the symptoms. It’s essential for individuals not to delay seeking the necessary care, as early intervention can significantly affect long-term prognoses.
Regular follow-ups with healthcare providers ensure that treatment plans remain effective and adjustments are made as needed. Patients should feel empowered to voice concerns regarding medication effectiveness, side effects, or new symptoms arising. Through ongoing communication, individuals can better navigate their pain management journey.
Ultimately, recognizing the appropriate times to seek professional help will help ensure that individuals receive timely, effective care. This proactive approach can dramatically improve the management of back head nerve pain and contribute to a healthier, more balanced life.