Head Hurts with Movement: Common Causes and Solutions
Table of contents
- Headaches often stem from musculoskeletal issues, particularly tension in the neck and back
- Cervical dysfunction is closely related to an increased frequency of headaches during activity
- 12% of the population experiences worsening migraines during physical activity
- Changes in facial pressure caused by sinusitis can trigger activity-related headaches
- Primary headaches exist independently, while secondary headaches indicate potential underlying diseases
- Different types of headaches exhibit various symptoms; migraines are often accompanied by nausea and light sensitivity
- Collecting a medical history combined with imaging tests is key to diagnosis
- Sudden severe headaches, especially with neurological symptoms, require immediate medical attention
- Lifestyle adjustments alongside medication yield better outcomes
- Maintaining hydration and balanced nutrition helps prevent headaches
- Activity-related headaches primarily include migraines and tension-type headaches
- Combining hot and cold compresses with hydration can effectively relieve activity-related headaches
- Frequent severe headaches require professional medical evaluation
- Managing stress and diet can significantly improve headache symptoms
- Good communication with the medical team is crucial for successful treatment
Analyzing Common Triggers of Activity-Related Headaches
Mechanisms of Influence from the Musculoskeletal System
When we maintain poor posture for long periods, the muscles in the neck and back can become continuously tense, like overstretched rubber bands. This mechanical pressure can cause localized soreness and, through nerve conduction, trigger referred headaches. Especially in patients with degenerative changes in the cervical spine, narrowing of the intervertebral foramen during head rotation may directly compress the nerve roots, causing electrifying shooting pain.
Clinical observations published in the \Headache and Pain Journal\ show that 68% of subjects receiving cervical manipulation reported a reduction of more than 50% in headache frequency. This indicates that targeted physical therapy can effectively break the vicious cycle of muscle tension-neural compression-exacerbated headaches.
Specific Conditions with Activity-Exacerbated Characteristics
Patients with migraines often feel severe movement of fluid within the cranium when climbing stairs or bending over. This phenomenon, referred to as head impact pain, is directly related to abnormal activation of the trigeminal vascular system. Recent neuroimaging studies have confirmed that metabolic activity in the nucleus raphe magnus of the brainstem abnormal rises during physical activity, leading to amplified pain signals.
For patients with sinusitis, changes in posture can feel like squeezing a water-filled rubber ball. When the thick secretions cannot be drained smoothly, the pressure in the closed cavity can spike dramatically. At this point, even simple nodding can make the pain in the frontal sinus region increase from 3 to 7 (based on a visual analog scale).
Differential Diagnosis of Headache Types
Essential Differences Between Primary and Secondary Headaches
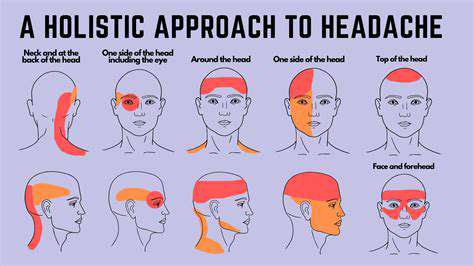
Primary headaches operate like an independent alarm system, occurring without the dependence on other diseases. These headaches often exhibit distinct characteristics: migraines prefer unilateral throbbing pain, while tension-type headaches feel like a tight band around the head.
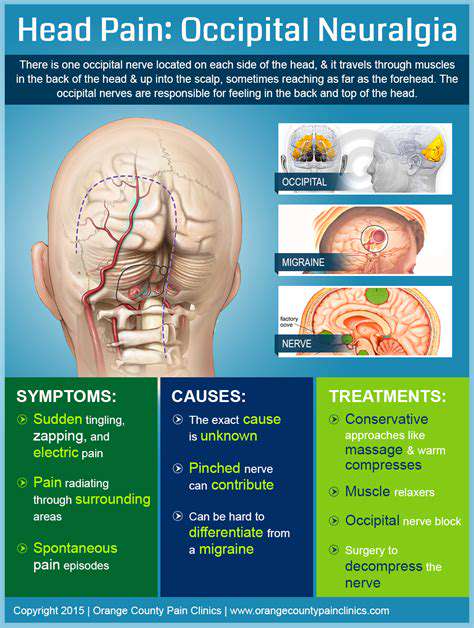
Secondary headaches serve more like a distress signal from the body. When treating patients with worsening headache symptoms, we remain highly alert. There have been cases where a patient's recurrent dull pain in the occipital area was ultimately diagnosed as a cerebellar tonsil herniation, reminding us never to overlook the underlying risks of headaches.
The Diagnostic Value of Symptom Combinations
In clinical practice, we pay special attention to the pattern of symptom combinations recorded in headache diaries. Migraine patients often describe experiencing a headache like a tidal wave after seeing flashes of light, while cluster headache patients may pinpoint an explosion of severe pain originating from behind the right eye precisely at 1 a.m.
Of particular concern, sudden headaches accompanied by fever may suggest meningitis, while headaches exacerbated by changes in posture must rule out low intracranial pressure. These subtle differences are often key breakthroughs for accurate diagnosis.
Application of Modern Diagnostic Technologies
In the neurology outpatient department, we utilize a stepwise diagnostic strategy: First, we identify suspicious directions through detailed history collection, then select specific auxiliary examinations. For young patients with new persistent headaches, magnetic resonance angiography effectively screens for cerebrovascular malformations; whereas for older patients with subacute headaches, a lumbar puncture is necessary to exclude chronic subdural hematoma.
Recent developments in artificial intelligence-assisted diagnostic systems have improved the recognition accuracy of migraines to 89% by analyzing patients' facial micro-expressions and speech features. This technological innovation is transforming traditional diagnostic models.
Warning Signs to Watch For
In clinical practice, we use the SNOOP mnemonic as a screening tool for danger signs:
- Systemic symptoms (fever, weight loss)
- Neurological signs (changes in consciousness, papilledema)
- Sudden severe pain (thunderclap headache)
- Age of onset >50 years
- Changes in pain pattern (frequency/intensity/nature changes)
Layered Treatment Strategies
Treatment options must follow the principle of individualization. For chronic migraines occurring more than four times a month, we recommend a stepwise medication approach: starting with supplements like magnesium and riboflavin, gradually transitioning to targeted medications like β-blockers or CGRP monoclonal antibodies.
For cervical headaches, we often employ a three-dimensional treatment mode: ultrasound-guided nerve blocks to alleviate acute pain, combined with suspension exercise training to improve neck muscle endurance, and finally using cognitive-behavioral therapy to correct poor posture habits.
Core Elements of Preventive Management
In preventing recurrence, we emphasize building a headache defense system:
- Biological rhythm management: fixed schedule to avoid sleep deprivation
- Stress buffering mechanism: daily 15 minutes of mindfulness meditation
- Nutrition support plan: supplementing ω-3 fatty acids and coenzyme Q10
- Environmental control: use of anti-blue light glasses and noise-canceling headphones
Home Strategies for Activity-Related Headaches

Identifying Headache Trigger Patterns
Patients are advised to establish a headache trigger log, recording the details of activities preceding each episode. A dance teacher discovered that headaches occurring after bending forward were actually due to compression of the vertebral artery. This self-observational skill can often help doctors more quickly pinpoint the cause.
Stepwise Relief Plan
We recommend a three-step relief method:1. Immediately stop the current activity and adopt box breathing (inhale for 4 seconds - hold for 4 seconds - exhale for 4 seconds)2. Choose a cold pack (for throbbing pain) or warm compress (for pressure pain) based on the nature of the pain3. Drink small sips of electrolyte-containing warm water, avoiding large gulps that may induce nausea
For cervical headaches, towel resistance training can be attempted: wrap a towel around the top of the head and pull forward and down with both hands while extending the neck backward, holding for 10 seconds as one set, three times a day.
The Key Role of Nutritional Intervention
Clinical nutrition research shows that continuous supplementation of 300mg coenzyme Q10 for eight weeks results in an average reduction of 30% in migraine episode frequency. It is recommended to include dark green vegetables, nuts, and deep-sea fish in daily diets. It is particularly important to note that some cheeses and processed meats may contain tyramine, which can become hidden triggers.
Principles for Developing Exercise Prescriptions
For patients with exercise-related headaches, we recommend a heart rate step-up training method: starting at 50% intensity of the maximum heart rate, increasing by 5% each week, allowing the cardiovascular system to gradually adapt. Additionally, it’s emphasized that dynamic stretching prior to exercise should sufficiently activate the neck and shoulder muscle groups, with immediate cold pack care following exercise.
When Professional Intervention is Needed
When home care fails to alleviate pain within two hours, or episodes exceed four times a month, it is advisable to initiate a professional medical evaluation. Especially watchful for unusual headaches, such as thunderclap pain that first occurs during sexual activity, which may indicate subarachnoid hemorrhage.
Warning Signs That Require Immediate Medical Attention
Danger Symptoms Identification Guidelines
We use the RED FLAGS mnemonic to help patients identify dangerous signals:
- Rapid onset (sudden severe headache)
- Elderly onset (new headache after age 50)
- Deficit symptoms (accompanied by neurological deficits)
- Fever/Systemic signs (fever/neck stiffness)
- Altered pattern (changes in pain pattern)
- Gravid state (new headache during pregnancy)
- Snellen acuity change (sudden vision drop)
Emergency Treatment Process Analysis
In the emergency department, physicians will apply the ABCs priority principle:
- Ensure stable Airway, Breathing, and Circulation
- Rapid neurological assessment (Glasgow coma scale)
- Emergency imaging (non-contrast CT to exclude bleeding)
- If necessary, lumbar puncture for pressure measurement and cerebrospinal fluid analysis
The Art of Doctor-Patient Communication
Effective history presentation should include the following elements:
- Location of pain (draw a diagram)
- Nature of pain (e.g. electric shock-like, stabbing)
- Accompanying symptoms (nausea, light sensitivity, etc.)
- Factors that relieve/exacerbate (posture, medication response)
- Temporal characteristics (heavier in the morning, lighter in the evening, etc.)